Abstract
Case Presentation
Renal Malakoplakia: A Diagnostic Challenge Presenting as a Subcapsular Collection despite Clinical Recovery
Mohammed Amine Elafari*, Mamad Ayoub, Mohammed Amine Bibat, Amine Slaoui, Tarik Karmouni, Abdelatif Koutani and Khalid Elkhader
Published: 09 April, 2026 | Volume 10 - Issue 1 | Pages: 032-038
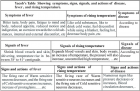
Background: Renal malakoplakia is a rare chronic granulomatous inflammatory disorder characterized by defective macrophage function. It typically occurs in immunocompromised patients with recurrent urinary tract infections. We present a case of renal malakoplakia in a diabetic patient who progressed to nephrectomy despite initial conservative management.
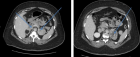
Case presentation: A 57-year-old female patient with a medical history of insulin-dependent type 2 diabetes mellitus was admitted to the hospital with symptoms including fever, left flank pain, and dysuria. A physical examination revealed a tender left lumbar mass. Laboratory investigations revealed a leukocytosis (16,500/mm³), elevated C-reactive protein (142 mg/L), and preserved renal function. A urine culture revealed the presence of multidrug-resistant Escherichia coli (>106CFU/mL). A subsequent Computed Tomography (CT) scan revealed an enlarged left kidney with a 9 × 6 cm multiloculated subcapsular collection, causing significant parenchymal compression, along with two non-obstructive inferior pole calculi. The initial management strategy encompassed ultrasound-guided percutaneous drainage and targeted antibiotic therapy, with the latter being contingent upon bacterial sensitivities. Notwithstanding the patient’s positive clinical recovery, Technetium-99m Dimercaptosuccinic Acid ((99m)Tc-DMSA) renal scintigraphy performed four weeks after the episode revealed a non-functional left kidney, exhibiting a 15% differential function. Following a multidisciplinary discussion, a total left nephrectomy was performed. A histopathological examination revealed extensive replacement of renal parenchyma by polymorphous inflammatory infiltrate with pathognomonic Michaelis-Gutmann bodies. These bodies are spherical, basophilic, perinuclear inclusions that demonstrate strong positivity for Periodic Acid-Schiff and Perls stains. The postoperative course was complicated by self-limited lymphorrhage. At the 3-month follow-up, the patient reported complete resolution of symptoms and remains under nephrological surveillance.
Conclusion: This case underscores the diagnostic challenges posed by renal malakoplakia, a condition that can present with a wide spectrum of mimics, including infectious and neoplastic processes. Early diagnosis and prolonged antibiotic therapy with agents capable of intracellular penetration may preserve renal function; however, nephrectomy remains necessary when irreversible parenchymal damage has occurred. Diabetes mellitus has been identified as a significant risk factor for malakoplakia development through impaired leukocyte function.
Read Full Article HTML DOI: 10.29328/journal.jcmei.1001046 Cite this Article Read Full Article PDF
Keywords:
Renal Malakoplakia, Michaelis-Gutmann Bodies, Diabetes Mellitus, Escherichia coli, Nephrectomy, Granulomatous Inflammation, Von Hansemann Cells, DMSA Scintigraphy
References
- Chaudhry AP, Satchidanand SK, Anthone R, Baumler RA, Gaeta JF. An unusual case of supraclavicular and colonic malakoplakia--a light and ultrastructural study. J Pathol. 1980;131(3):193-208. Available from: https://pubmed.ncbi.nlm.nih.gov/6253612/
- Dobyan DC, Truong LD, Eknoyan G. Renal malacoplakia reappraised. Am J Kidney Dis. 1993;22(2):243-52. Available from: https://pubmed.ncbi.nlm.nih.gov/8352248/
- Mitchell MA, Markovitz DM, Killen PD, Braun DK. Bilateral renal parenchymal malacoplakia presenting as fever of unknown origin: case report and review. Clin Infect Dis. 1994;18(5):704-18. Available from: https://pubmed.ncbi.nlm.nih.gov/7915547/
- Zhang Y, Byrnes K, Lam-Himlin D, Pittman M, Pezhouh M, Gonzalez RS, et al. Gastrointestinal malakoplakia: clinicopathologic analysis of 26 cases. Am J Surg Pathol. 2020;44(9):1251-1258. Available from: https://pubmed.ncbi.nlm.nih.gov/32301754/
- Teeters JC, Betts R, Ryan C, Huether J, Elias K, Hartmann D, et al. Rectal and cutaneous malakoplakia in an orthotopic cardiac transplant recipient. J Heart Lung Transplant. 2007;26(4):411-3. Available from: https://pubmed.ncbi.nlm.nih.gov/17403486/
- Chou SC, Wang JS, Tseng HH. Malacoplakia of the ovary, fallopian tube, and uterus: a case associated with diabetes mellitus. Pathol Int. 2002;52(12):789-93. Available from: https://pubmed.ncbi.nlm.nih.gov/12588449/
- Chen CS, Lai MK, Hsueh S, Hwang TL, Chuang CK. Renal malacoplakia with secondary hepato-duodenal involvement. J Urol. 1994;151(4):982-5. Available from: https://pubmed.ncbi.nlm.nih.gov/8126844/
- Tam VK, Kung WH, Li R, Chan KW. Renal parenchymal malacoplakia: a rare cause of ARF with a review of recent literature. Am J Kidney Dis. 2003;41(6):E13-E17. Available from: https://pubmed.ncbi.nlm.nih.gov/12776305/
- Fatola A, Johnson BC, Walsh L, Fang D, White MJ, Le D, et al. A very complicated UTI: malakoplakia following E. coli urinary tract infection. BMC Nephrol. 2024;25(1):200. Available from: https://pubmed.ncbi.nlm.nih.gov/38890600/
- Chaudhry N, Vazzano J, Parwani A. Case study: malakoplakia of the bladder. Pathol Res Pract. 2022;237:153852. Available from: https://pubmed.ncbi.nlm.nih.gov/35878530/
- Pan Y, Hong YC, Shih HJ, Chang C, Huang S, Wu S, et al. Malakoplakia and xanthogranulomatous pyelonephritis treated with nephrectomy: a case report. Medicine (Baltimore). 2021;100(36):e27137. Available from: https://pubmed.ncbi.nlm.nih.gov/34516505/
- Wang Z, Ren J. Clinical analysis of renal failure caused by malakoplakia: a case report and literature review. Front Med (Lausanne). 2022;9:770731. Available from: https://www.researchgate.net/publication/358987906_Clinical_Analysis_of_Renal_Failure_Caused_by_Malakoplakia_A_Case_Report_and_Literature_Review
Figures:
Similar Articles
Recently Viewed
-
Low Level Light Therapy (LLLT): Penetration and PhotobiomodulationCecilia Young*,Cheuk Lam Mak. Low Level Light Therapy (LLLT): Penetration and Photobiomodulation. J Oral Health Craniofac Sci. 2017: doi: 10.29328/journal.johcs.1001015; 2: 080-082
-
Type 2 diabetes and cancerSnobia Munir*,Samreen Riaz. Type 2 diabetes and cancer. Ann Clin Endocrinol Metabol. 2020: doi: 10.29328/journal.acem.1001012; 4: 001-006
-
Renal Malakoplakia: A Diagnostic Challenge Presenting as a Subcapsular Collection despite Clinical RecoveryMohammed Amine Elafari*,Mamad Ayoub,Mohammed Amine Bibat,Amine Slaoui,Tarik Karmouni,Abdelatif Koutani,Khalid Elkhader. Renal Malakoplakia: A Diagnostic Challenge Presenting as a Subcapsular Collection despite Clinical Recovery. J Clin Med Exp Images. 2026: doi: 10.29328/journal.jcmei.1001046; 10: 032-038
-
Medicinal plant Potentilla fulgens and its effect in vitro against Fasciola giganticaPradeep Kumar*. Medicinal plant Potentilla fulgens and its effect in vitro against Fasciola gigantica. Insights Clin Cell Immunol. 2021: doi: 10.29328/journal.icci.1001018; 5: 004-007
-
Precision and personalized vaccines needed to face COVID-19 pandemicDahmani Fathallah M*. Precision and personalized vaccines needed to face COVID-19 pandemic. Insights Clin Cell Immunol. 2021: doi: 10.29328/journal.icci.1001017; 5: 003-003
Most Viewed
-
Physical Performance in the Overweight/Obesity Children Evaluation and RehabilitationCristina Popescu, Mircea-Sebastian Șerbănescu, Gigi Calin*, Magdalena Rodica Trăistaru. Physical Performance in the Overweight/Obesity Children Evaluation and Rehabilitation. Ann Clin Endocrinol Metabol. 2024 doi: 10.29328/journal.acem.1001030; 8: 004-012
-
Hypercalcaemic Crisis Associated with Hyperthyroidism: A Rare and Challenging PresentationKarthik Baburaj*, Priya Thottiyil Nair, Abeed Hussain, Vimal MV. Hypercalcaemic Crisis Associated with Hyperthyroidism: A Rare and Challenging Presentation. Ann Clin Endocrinol Metabol. 2024 doi: 10.29328/journal.acem.1001029; 8: 001-003
-
Effects of dietary supplementation on progression to type 2 diabetes in subjects with prediabetes: a single center randomized double-blind placebo-controlled trialSathit Niramitmahapanya*,Preeyapat Chattieng,Tiersidh Nasomphan,Korbtham Sathirakul. Effects of dietary supplementation on progression to type 2 diabetes in subjects with prediabetes: a single center randomized double-blind placebo-controlled trial. Ann Clin Endocrinol Metabol. 2023 doi: 10.29328/journal.acem.1001026; 7: 00-007
-
Exceptional cancer responders: A zone-to-goDaniel Gandia,Cecilia Suárez*. Exceptional cancer responders: A zone-to-go. Arch Cancer Sci Ther. 2023 doi: 10.29328/journal.acst.1001033; 7: 001-002
-
Ectopic adrenal tissue at the spermatic cordAbdallah Chaachou,Nizar Cherni,Wael Ferjaoui*,Mohamed Dridi,Samir Ghozzi. Ectopic adrenal tissue at the spermatic cord. J Clin Med Exp Images. 2022 doi: 10.29328/journal.jcmei.1001024; 6: 001-002

If you are already a member of our network and need to keep track of any developments regarding a question you have already submitted, click "take me to my Query."