Early Online (Volume - 10 | Issue - 1)
Penile Fracture: The “Cracking” Sound and Intra-operative Tunica Albuginea Repair
Published on: 21st January, 2026
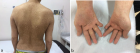
Penile fracture is a rare urological emergency typically characterized by an audible “cracking” sound, immediate detumescence, and rapid penile swelling following trauma to an erect penis. We present clinical and intra-operative images of a 37-year-old man with a proximal tunica albuginea tear confirmed at urgent exploration and repaired with absorbable sutures. Early surgical exploration with hematoma evacuation and primary repair remains the preferred approach to reduce long-term complications such as penile curvature and erectile dysfunction.
Obstructive Pyelonephritis Due to Postoperative Ureteral Stricture: A Case Report
Published on: 9th February, 2026
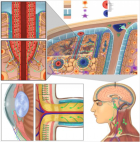
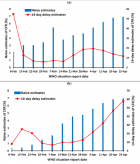
Iatrogenic ureteral injury is an uncommon but potentially severe complication of abdominopelvic surgery. When not identified intraoperatively, it may present days to weeks later with flank pain, fever, urinary tract infection, and imaging evidence of obstruction. Early recognition and timely urinary diversion are essential to prevent sepsis and preserve renal function.A 65-year-old patient underwent elective resection of an abdominal mass; pathology confirmed schwannoma. On postoperative day 15, the patient developed left flank pain and fever. Laboratory tests showed leukocytosis (WBC 15,000/mm³) and elevated C-reactive protein (150 mg/L); urine culture grew Escherichia coli. Contrast-enhanced CT demonstrated left hydronephrosis without stones, suggesting postoperative ureteral obstruction. Retrograde double-J stenting was attempted but failed. Urgent percutaneous nephrostomy achieved decompression with clinical improvement under targeted antibiotics. Definitive exploration revealed a 1 cm stricture of the lumbar ureter, managed by segmental resection and tension-free spatulated termino-terminal ureteroureterostomy over an internal stent. Postoperative recovery was uncomplicated; the stent was removed after 3 weeks. Follow-up ultrasound showed no persistent pelvicalyceal dilatation.Delayed ureteral obstruction should be suspected in postoperative patients presenting with flank pain, fever, and hydronephrosis. When retrograde stenting fails in the setting of infection, percutaneous nephrostomy provides rapid decompression and source control, allowing delayed definitive reconstruction. For short-segment proximal or mid-ureter strictures, ureteroureterostomy remains a reliable option when performed according to reconstructive principles.
Stone on the Mesh: Intravesical Erosion after Laparoscopic Promontofixation-A Hidden Cost of Durability
Published on: 19th February, 2026
Intravaginal erosion of synthetic mesh after laparoscopic promontofixation(sacrocolpopexy) is an uncommon but clinically relevant late complication. When mesh becomes exposed within the bladder, it may function as a persistent foreign body, encouraging chronic inflammation, bacterial colonization, recurrent lower urinary tract symptoms, and progressive encrustation that can culminate in bladder stone formation. We report a 60-year-old woman with a history of laparoscopic promontofixation using standard polypropylene mesh performed approximately five years earlier. She presented with progressive urinary symptoms. Bladder ultrasound demonstrated an intravesical calculus, and diagnostic cystoscopy confirmed a bladder stone developing on exposed intravesical mesh fibers, consistent with intravesical mesh erosion. Endoscopic management was performed with cystolithotripsy followed by section/resection and removal of the exposed intravesical mesh to eliminate the lithogenic nidus, with a favorable outcome. In women with prior promontofixation presenting with bladder stones, recurrent urinary tract infections, hematuria, or persistent irritative urinary symptoms, intravesical mesh erosion must be considered. Cystoscopy is essential for diagnosis because imaging may identify the stone but not the underlying foreign-body etiology, and definitive treatment requires both stone clearance and elimination of intravesical foreign material to prevent recurrence.
Febrile Lumbar Pain Revealing a Massive Collection: Complicated Psoas Abscess Managed Surgically
Published on: 5th March, 2026
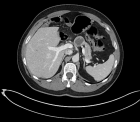
Psoas abscess is a rare but potentially life-threatening condition with non-specific clinical manifestations. The condition may be primary or secondary, depending on whether it has an underlying cause. The condition may be diagnosed with the help of imaging studies, especially contrast-enhanced computed tomography (CT).A 55-year-old female patient with a history of treated hypertension presented with a 15-day history of fever and left-sided low back pain. Her laboratory parameters showed a high leukocyte count of 22,000 cells/mm³ and elevated levels of C-reactive protein (367 mg/L). Her renal functions were within normal limits, and the urine culture was negative. Contrast-enhanced CT revealed a large left-sided intra-abdominal fluid collection extending from the diaphragm to the left iliac fossa, measuring 66 x 305 mm with air bubbles. The collection also showed a left-sided intramuscular psoas collection of 66 x 50 x 131 mm. The patient received intravenous broad-spectrum antibiotics (third-generation cephalosporin, aminoglycoside, and metronidazole). The patient underwent mini-lumbotomy, and nearly 1 liter of pus was drained. The patient’s postoperative course was satisfactory with complete resolution of symptoms. The histopathological examination showed non-specific changes.Psoas abscess should be suspected in patients with febrile low back pain and inflammatory syndrome. Contrast-enhanced CT scans are essential for diagnosis and assessment of the extent of disease. In complicated cases with large abscess formation, early surgical drainage along with appropriate antibiotics will provide the best outcome.This case highlights the importance of early diagnosis and adapted management for successfully navigating the complexities associated with this condition.
Bilateral Severe Encrustation of Long-Term Indwelling Double-J Stents in a Young Non-Lithiasic Patient
Published on: 16th March, 2026
Ureteral double-J stents are a commonly used device in urological practice to allow urinary drainage, avoid ureteral obstruction processes, and protect the upper urinary tract after surgical procedures. However, long indwelling time may give rise to numerous complications, such as infection, migration, and fragmentation of the stent, especially encrustation. Encrustation of stents is a well-known complication that has been closely related to the time active of the stent and can cause significant morbidity if not timely addressed. In severe cases, abundant mineral deposition can result in the development of large calculi encasing the stent and rarely progress to staghorn stones. These cases may pose challenges in terms of the extraction of the stent and may result in complex endourological intervention. The encrustation likelihood is substantially higher if stents are left forgotten or remain in place longer than the advised period. Most patients with heavily encrusted stents have symptoms including flank pain, urinary tract infection, hematuria, or obstructive uropathy, but can present without any symptoms, and this can delay the diagnosis.
Not Every Bladder Mass Is Malignant: A Case of Inverted Urothelial Papilloma in a Young Adult
Published on: 30th March, 2026
Inverted Urothelial Papilloma (IUP) is an unusual variety of urothelial tumors that typically occurs in adults, with a predominance in males. The definitive diagnosis of IUP relies on histopathological examination, as the clinical presentation and endoscopic appearance are non-specific. The recommended treatment for IUP includes the complete transurethral resection, with some controversy regarding the need for cystoscopic follow-up. In this case, we present an atypical instance of IUP in a 21-year-old male patient, diagnosed with gross hematuria and irritative lower urinary tract symptoms. A clinical assessment revealed a 3.0 × 2.6 cm intravesical mass. The definitive diagnosis was confirmed histopathologically and further substantiated by immunohistochemistry, which demonstrated low expression of p53 and Ki-67, effectively ruling out malignancy. This case underscores the diagnostic challenges posed by bladder masses in young adults, emphasizing the necessity of integrating morphological and immunohistochemical findings to prevent overdiagnosis of urothelial carcinoma. The paper focuses on the diagnostic approach and management of this rare condition in the young male population.
Adult Bladder Exstrophy with Premalignant Changes Following Failed Reconstruction: A Case Report
Published on: 1st April, 2026
Background: Bladder exstrophy is a rare congenital abnormality that is usually managed with multiple surgical interventions. Long-term consequences include recurrent urinary tract infections, bladder stones, fistulae, and metaplastic changes with malignant potential.Case Presentation: We present a case of a 21-year-old male with a history of failed childhood surgeries for bladder exstrophy who presented with a vesicocutaneous fistula and a 7 cm bladder stone. He underwent an open cystolithotomy with bladder augmentation and creation of a Benchekroun continent valve. However, the patient developed recurrent fistulae due to poor tissue quality. Histopathological examination confirmed early squamous metaplasia in the bladder mucosa. After discussion in a multidisciplinary meeting, the patient underwent a radical cystectomy with ileal conduit urinary diversion using the Bricker technique. He is doing well at 3 months with no evidence of any complication.Conclusion: This case illustrates the difficulties encountered in managing adult patients with bladder exstrophy and failed reconstructions. The presence of squamous metaplasia, poor bladder tissue, and recurrent complications all contributed to the decision for radical cystectomy. It is important to recognize these changes and address them appropriately in a timely manner to prevent further complications and possible malignant changes.
Burch Colposuspension for Female Stress Urinary Incontinence: A Narrative Review of Contemporary Evidence and Urodynamic Perspectives
Published on: 9th April, 2026
Background: Burch colposuspension is a mesh-free retropubic urethropexy for female stress urinary incontinence (SUI). Amidst increasing scrutiny of synthetic materials, re-evaluating its long-term efficacy and urodynamic profile is essential. Objective: To review contemporary evidence regarding the urodynamic mechanisms, clinical efficacy, and safety profile of the Burch procedure. Methods: A comprehensive literature search was conducted across PubMed, Cochrane Library, and Google Scholar for studies published up to 2025. We included randomized controlled trials, meta-analyses, and long-term cohort studies focusing on Burch colposuspension compared to midurethral slings and autologous slings. Results: Open colposuspension achieves objective cure rates of 68.9%–88% in the first year, with approximately 70% maintaining continence at five years. Long-term studies (mean 13.1 years) show comparable efficacy to midurethral slings (83% vs. 85%). The procedure restores continence by enhancing pressure transmission to the proximal urethra without altering intrinsic sphincter function. While autologous fascial slings offer higher stress-specific success (66% vs. 49%), they carry significantly higher risks of voiding dysfunction requiring reoperation (6.1% vs. 0%). Common complications of Burch include de novo overactive bladder (3%–4.1%) and a higher risk of posterior compartment prolapse (3.3%) compared to slings. Conclusions: Burch colposuspension remains a gold-standard, mesh-free intervention for women with urethral hypermobility, especially those undergoing concurrent abdominal surgery. It provides a durable, safe alternative to synthetic slings with a lower risk of obstructive voiding dysfunction, though patients should be counseled regarding potential long-term pelvic organ prolapse.
Renal Malakoplakia: A Diagnostic Challenge Presenting as a Subcapsular Collection despite Clinical Recovery
Published on: 9th April, 2026
Background: Renal malakoplakia is a rare chronic granulomatous inflammatory disorder characterized by defective macrophage function. It typically occurs in immunocompromised patients with recurrent urinary tract infections. We present a case of renal malakoplakia in a diabetic patient who progressed to nephrectomy despite initial conservative management.Case presentation: A 57-year-old female patient with a medical history of insulin-dependent type 2 diabetes mellitus was admitted to the hospital with symptoms including fever, left flank pain, and dysuria. A physical examination revealed a tender left lumbar mass. Laboratory investigations revealed a leukocytosis (16,500/mm³), elevated C-reactive protein (142 mg/L), and preserved renal function. A urine culture revealed the presence of multidrug-resistant Escherichia coli (>106CFU/mL). A subsequent Computed Tomography (CT) scan revealed an enlarged left kidney with a 9 × 6 cm multiloculated subcapsular collection, causing significant parenchymal compression, along with two non-obstructive inferior pole calculi. The initial management strategy encompassed ultrasound-guided percutaneous drainage and targeted antibiotic therapy, with the latter being contingent upon bacterial sensitivities. Notwithstanding the patient’s positive clinical recovery, Technetium-99m Dimercaptosuccinic Acid ((99m)Tc-DMSA) renal scintigraphy performed four weeks after the episode revealed a non-functional left kidney, exhibiting a 15% differential function. Following a multidisciplinary discussion, a total left nephrectomy was performed. A histopathological examination revealed extensive replacement of renal parenchyma by polymorphous inflammatory infiltrate with pathognomonic Michaelis-Gutmann bodies. These bodies are spherical, basophilic, perinuclear inclusions that demonstrate strong positivity for Periodic Acid-Schiff and Perls stains. The postoperative course was complicated by self-limited lymphorrhage. At the 3-month follow-up, the patient reported complete resolution of symptoms and remains under nephrological surveillance.Conclusion: This case underscores the diagnostic challenges posed by renal malakoplakia, a condition that can present with a wide spectrum of mimics, including infectious and neoplastic processes. Early diagnosis and prolonged antibiotic therapy with agents capable of intracellular penetration may preserve renal function; however, nephrectomy remains necessary when irreversible parenchymal damage has occurred. Diabetes mellitus has been identified as a significant risk factor for malakoplakia development through impaired leukocyte function.

If you are already a member of our network and need to keep track of any developments regarding a question you have already submitted, click "take me to my Query."